Table of Contents
Understanding Urinary Incontinence in Fort Lauderdale
Understanding urinary incontinence in Fort Lauderdale starts with recognizing its types and underlying causes. Urinary incontinence is the involuntary leakage of urine, a condition that affects millions of women across all ages. The three main types are stress urinary incontinence, urge incontinence (often called overactive bladder), and mixed incontinence, which is a combination of both.
A variety of factors familiar to many women in our community can contribute to bladder control problems. Pregnancy and childbirth may weaken pelvic floor muscles, while menopause reduces estrogen levels that support urethral strength. Excess weight, pelvic surgery, and the natural changes of aging also increase risk. The Office on Women's Health reports that more than 4 in 10 women over age 65 experience urinary incontinence, though it can affect younger women as well. It is essential to understand that urinary incontinence is not a normal part of aging--and it is treatable. For women in our community, understanding these risk factors empowers them to seek the care they deserve.
Recognizing the specific type of incontinence is a vital first step toward relief. Women in Fort Lauderdale can access expert urinary incontinence treatment at Dr. Anghel's practice, where we deliver expert, attentive care and combine advanced medical approaches with personalized support. Next, we explore how lifestyle factors and specific conditions can trigger or worsen symptoms.
The Fundamentals of Urinary Incontinence: Causes and Types
Urinary incontinence in Fort Lauderdale is a common condition that affects many women, yet it is not a normal part of aging. It refers to involuntary urine leakage, ranging from a few drops to complete bladder emptying. The two most common types--stress incontinence and urge incontinence--have distinct causes and triggers, and identifying which type you have is the first step toward effective treatment.
Stress Incontinence
According to Mayo Clinic, stress incontinence occurs when physical pressure on the bladder--such as coughing, sneezing, or exercise--overcomes weakened pelvic floor muscles, causing urine leakage. Common risk factors include pregnancy, childbirth, menopause, obesity, and age-related muscle loss. Neurological disorders such as multiple sclerosis or stroke can also impair bladder control. Many women first notice symptoms after pregnancy or during menopause when estrogen levels decline, weakening pelvic tissues. High-impact activities and obesity add chronic pressure on the bladder. First-line approaches for stress incontinence treatment focus on strengthening the pelvic floor. The American College of Obstetricians and Gynecologists (ACOG) recommends Kegel exercises, lifestyle modifications, and physical therapy. Physical therapists teach proper techniques to engage the right muscles, and avoiding bladder irritants like caffeine can also help reduce leakage.
Urge Incontinence
Mayo Clinic explains that urge incontinence, often called overactive bladder, results from sudden involuntary bladder contractions that create an urgent need to urinate, often leading to leakage before reaching the bathroom. The sensation can be so overwhelming it disrupts daily activities and sleep. Common triggers include cold weather, running water, anxiety, or sudden position changes. Underlying causes range from neurological conditions like multiple sclerosis and Parkinson's disease to diabetes, constipation, and bladder irritants. For men, an enlarged prostate can contribute. For overactive bladder treatment, behavioral therapies are first-line. ACOG guidelines emphasize bladder training to normalize urination intervals and medications that calm bladder spasms. Neuromodulation therapies are reserved for more persistent cases. Keeping a bladder diary and avoiding caffeine and alcohol can also help reduce symptoms.
To highlight these differences, the following table compares stress and urge incontinence:
| Feature | Stress Incontinence | Urge Incontinence |
|---|---|---|
| Cause | Physical pressure on the bladder (coughing, sneezing, exercise) | Involuntary bladder contraction (sudden, strong urge) |
| Common Symptoms | Leakage with movement, laughing, lifting | Needing to urinate urgently; leakage before reaching the bathroom |
| Triggers | Physical activity, coughing, sneezing, exercise | Cold weather, running water, anxiety, sudden changes in position |
| Common First-Line Treatments | Pelvic floor exercises, lifestyle changes, physical therapy | Bladder training, medications, neuromodulation |
Understanding which type you have guides the most effective treatment approach. While stress and urge incontinence differ, many women experience mixed incontinence--a combination of both. Both conditions are highly treatable with a range of options, from pelvic floor therapy to medication. Our board-certified urogynecologists at First Class OBGYN provide expert diagnosis and personalized care. For compassionate, expert treatment, consider Urinary Incontinence Treatment In Fort Lauderdale at our practice.
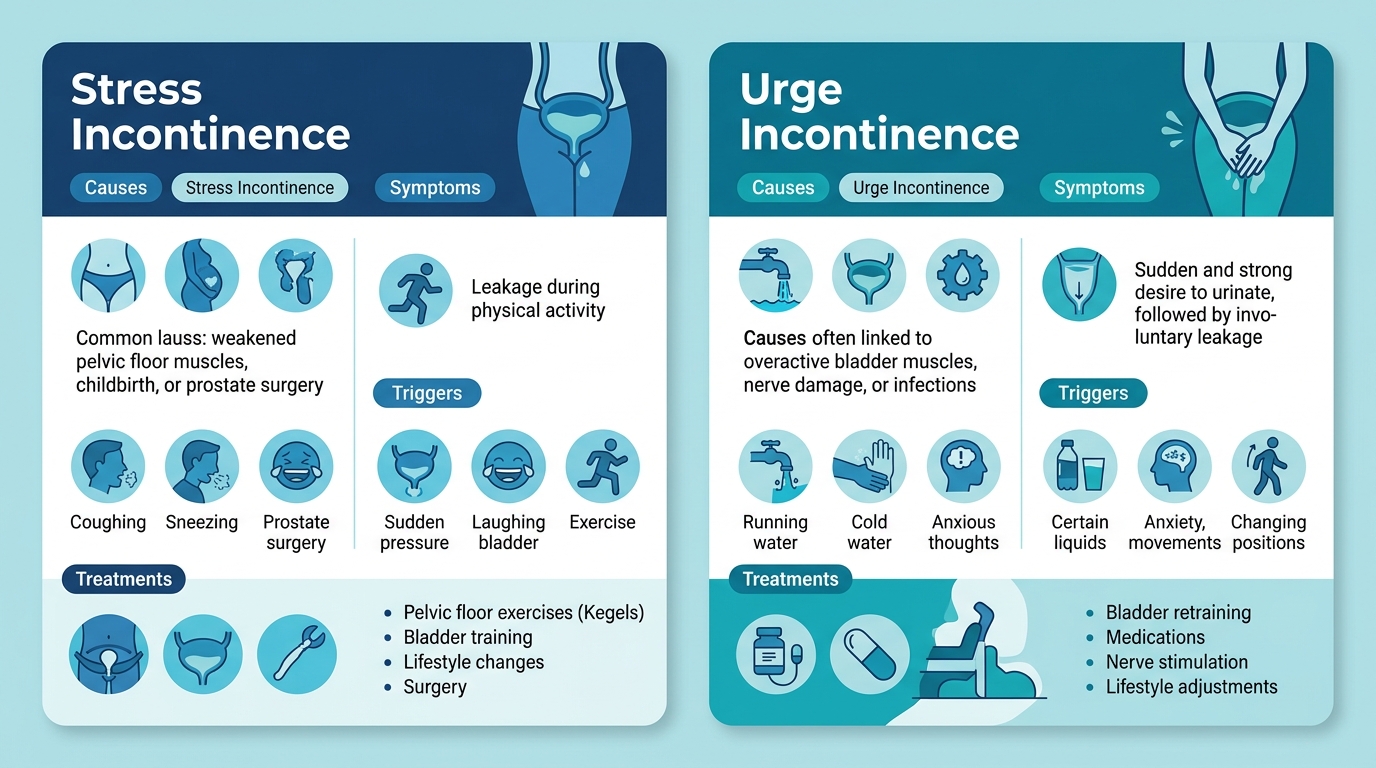
Comparison infographic of stress vs urge incontinence with triggers and treatments
Stress Incontinence vs. Overactive Bladder: Key Differences and Treatment Approaches
For women in Fort Lauderdale seeking answers about urinary incontinence, our team at First Class OBGYN provides expert and attentive care. Urinary Incontinence Fort Lauderdale--whether stress, urge, or mixed--can be effectively managed when correctly diagnosed. Understanding the type of incontinence you have is the first step toward effective treatment.
Understanding Stress Incontinence
Stress incontinence results from weakened support of the urethra, most commonly due to urethral hypermobility or intrinsic sphincter deficiency. According to the Urology Care Foundation, childbirth, aging, and pelvic surgery are frequent causes. Leakage occurs with physical activities that increase abdominal pressure--such as coughing, laughing, or exercising--and typically does not involve a preceding urge to urinate. Stress incontinence treatment often begins with pelvic floor exercises and behavioral strategies; our team's expert and attentive care ensures each woman receives a tailored plan from the outset.
Understanding Overactive Bladder (Urge Incontinence)
Overactive bladder (OAB) is defined by involuntary detrusor muscle contractions that produce a sudden, intense need to void. Mayo Clinic notes that neurological conditions like Parkinson's disease or stroke can trigger OAB, though many cases remain idiopathic. Unlike stress incontinence, physical activity does not directly cause leakage; instead, patients experience urgency and frequency, often with leakage before reaching the toilet. While mild symptoms may improve with lifestyle modifications, our overactive bladder treatment plans include medication and advanced therapies like InterStim neuromodulation, always guided by the safest and most effective care.
Non-Surgical Treatment Options for Both Types
Many women achieve significant improvement without surgery. Behavioral therapy--including bladder training and timed voiding--is particularly effective for urge incontinence, as confirmed by the Urology Care Foundation. Pelvic floor biofeedback uses sensors to teach correct Kegel exercises, offering a key stress incontinence treatment. For some, mechanical devices such as pessaries provide additional support. Medications also play a role, with options that relax the bladder or tighten the sphincter. Our team prioritizes the safest and most effective care, combining evidence-based approaches to reduce symptoms and restore confidence.
The following table compares common non-surgical approaches our team recommends.
| Treatment Type | How It Works | Best For | Considerations |
|---|---|---|---|
| Behavioral Therapy | Bladder training, scheduled voiding, fluid management | Urge incontinence; mild to moderate symptoms | Requires commitment; effective when combined with other therapies |
| Medications | Relax bladder muscle or tighten urethral sphincter | Overactive bladder; some stress incontinence options | Possible side effects (dry mouth, constipation); not always covered |
| Pelvic Floor Biofeedback | Uses sensors to teach correct pelvic floor muscle exercise | Stress incontinence; patients struggling with Kegels alone | Often covered by insurance; requires special equipment |
| Mechanical Devices (e.g., pessary) | Vaginal support device that lifts the bladder neck | Stress incontinence; women who cannot undergo surgery | Must be fitted by provider; periodic cleaning required |
Medications for Incontinence: What You Should Know
Medication choices vary markedly between the two conditions. For overactive bladder, anticholinergics such as oxybutynin and beta-3 agonists like mirabegron are first-line agents. Mayo Clinic reports that these drugs relax the bladder muscle but may cause dry mouth, constipation, and blurred vision. Duloxetine, an off-label option for stress incontinence, provides modest improvement yet carries potential side effects including urinary retention. We help women weigh benefits and risks, ensuring that every treatment aligns with their health profile. For those who do not achieve adequate relief with non-surgical methods, advanced surgical options--such as our da Vinci robotic-assisted procedures--offer the least invasive gynecologic surgery available today.
Practical Steps to Manage Urinary Incontinence: Pelvic Floor Exercises and Lifestyle Changes
Now that you understand the types of urinary incontinence, here are practical steps you can take at home to regain control. If you are facing urinary incontinence in Fort Lauderdale, these evidence-based strategies form the foundation of effective, non-invasive treatment. At First Class OBGYN, we believe in empowering you with the tools and knowledge to improve your daily life.
Pelvic Floor Exercises: Mastering Kegels and Beyond
Identifying your pelvic floor muscles is the first step. The "stop the urine stream" test can help locate them, but avoid doing it regularly as it may lead to incomplete bladder emptying. Once located, proper Kegel technique involves tightening the muscles--as if holding back gas or urine--for 5 to 10 seconds, then relaxing fully for 10 seconds. Aim for 10 to 15 repetitions, three times daily. According to Mayo Clinic guidelines, consistency with Kegels is essential and can lead to noticeable improvement within a few weeks. For those who struggle with technique or need more intensive strengthening, advanced methods such as biofeedback and electrical stimulation offer higher effectiveness. The table below compares these approaches to help you choose the best starting point.
| Method | Description | Effectiveness | How to Get Started |
|---|---|---|---|
| Kegels (Self-Guided) | Voluntary contractions of pelvic floor muscles | Moderate if done correctly; high drop-off rate | Count to 5 while tightening; release. 10 reps, 3x/day. |
| Biofeedback Therapy | Uses a sensor to show muscle activity in real time | High - learns correct technique quickly | Visit a pelvic floor physical therapist or provider with biofeedback equipment |
| Electrical Stimulation | Mild electrical pulses to contract pelvic floor muscles | High for urge incontinence; moderate for stress | Supervised by a provider; can be done at home with a device |
| Pelvic Floor Physical Therapy | One-on-one sessions with a specially trained PT | Very high - tailored to individual needs | Get a referral or find a therapist who specializes in women's health |
Bladder Training Techniques
Bladder training is a cornerstone of overactive bladder treatment and helps retrain your bladder to hold urine longer. Start by scheduling toilet trips every 2 to 3 hours, rather than waiting for an urge. Gradually extend the interval by 15-30 minutes each week. When urgency strikes, use suppression strategies:
- Deep breathing: Slow, controlled breaths calm the bladder reflex.
- Mental distraction: Focus on a task or count backward to shift attention.
- Quick pelvic floor clenches: A series of rapid Kegels can dampen the urge.
Lifestyle Modifications to Reduce Leakage
Simple daily changes can dramatically reduce leakage severity. We recommend a comprehensive approach:
- Diet: Limit caffeine to one cup per day and reduce acidic and spicy foods that can irritate the bladder. Avoid alcohol, which may increase urine production.
- Fluid management: Spread fluid intake throughout the day; avoid drinking large amounts before bedtime.
- Weight management: For those who are overweight, losing just 5-10% of body weight can lower urine leakage significantly.
- Smoking cessation: Quitting reduces coughing and bladder irritation; seek cessation support through your provider.
- Constipation relief: Treat constipation with a high-fiber diet and adequate fluids, as straining puts pressure on the pelvic floor.
Advanced Treatment Options and When to Seek Urogynecologic Care
If conservative measures have not provided adequate relief, advanced minimally invasive procedures may offer a more definitive solution. For residents in Fort Lauderdale experiencing urinary incontinence, understanding these options is an important step toward regaining confidence and comfort.
| Procedure | Target Problem | Recovery | Success Rate |
|---|---|---|---|
| Sling Surgery (e.g., mid-urethral sling) | Stress incontinence | 2-4 weeks light activity; full recovery 6 weeks | 80-95% improvement in leakage |
| Sacral Neuromodulation (InterStim) | Urge incontinence / overactive bladder | Day procedure; 1-2 weeks post-op adjustment | 70-80% significant improvement |
| Botox Injections (into bladder muscle) | Urge incontinence / overactive bladder | Minimal; effect lasts 6-9 months | 50-70% reduction in urgency episodes |
| Laser Therapy (e.g., MonaLisa Touch) | Vaginal atrophy, mild stress incontinence | No downtime; 3 sessions recommended | 60-75% improvement in symptoms |
Frequently Asked Questions About Urinary Incontinence
What treatment options for urinary incontinence are available in Fort Lauderdale?
Urinary incontinence is involuntary loss of urine, with stress, urge, and mixed as main types. We offer personalized care.
What causes stress incontinence?
According to the American College of Obstetricians and Gynecologists, stress incontinence occurs when pelvic floor muscles weaken. Stress incontinence treatment may involve pelvic floor exercises and minimally invasive procedures.
How is overactive bladder managed?
Overactive bladder (urge incontinence) causes sudden urges. We provide overactive bladder treatment including bladder training, pelvic floor therapy, and InterStim therapy.
Can urinary incontinence be treated without surgery?
Most cases improve without surgery through conservative care. We emphasize non-surgical approaches first, offering advanced minimally invasive options when needed.
Your Path to Better Bladder Health in Fort Lauderdale
If you're seeking relief from urinary incontinence in Fort Lauderdale, our practice provides a personalized path to lasting bladder control. We offer targeted treatments including stress incontinence treatment and overactive bladder treatment, with advanced options like InterStim therapy and Botox injections for the bladder. Our board-certified specialist provides expert and attentive care at every stage of a woman's life. Contact our Fort Lauderdale office to start your journey toward better bladder health.














