Table of Contents
Understanding Pelvic Floor Therapy in Fort Lauderdale
According to the Office on Women's Health, pelvic floor disorders affect millions of women, causing symptoms like urinary leakage and pelvic pressure. Pelvic floor therapy in Fort Lauderdale is a specialized physical therapy that uses manual techniques, biofeedback, and targeted exercises to strengthen and coordinate the pelvic floor muscles, improving support for the pelvic organs and alleviating symptoms. Pelvic floor dysfunction can lead to a range of challenges, from urinary incontinence to pelvic organ prolapse, and our therapy aims to restore function and comfort. For women in Fort Lauderdale, Pelvic Floor Therapy offers a non-surgical path to relief that is recommended by gynecologists and urogynecologists as a first-line conservative treatment. Our team at First Class OBGYN provides Expert and attentive care for every stage of a woman's life, integrating pelvic floor therapy into our comprehensive urogynecological services.
For women dealing with bladder control issues or pelvic pain, pelvic floor therapy in Fort Lauderdale provides a proven nonsurgical option. The American College of Obstetricians and Gynecologists (ACOG) recommends pelvic floor therapy as a first-line approach for conditions such as pelvic organ prolapse and stress or urge urinary incontinence. At First Class OBGYN, we offer comprehensive urogynecological care that includes a thorough evaluation, bladder training, personalized pelvic floor exercises, and advanced therapies like InterStim neuro-modulation and Botox injections for the bladder when conservative measures are not enough. We combine evidence-based protocols with the safest and most effective care to address pelvic floor dysfunction, helping women regain control and comfort. Our team tailors pelvic floor therapy plans to each woman's unique needs, helping her feel comfortable and confident. For specialized care, turn to our Urogynecology Fort Lauderdale team, which integrates pelvic floor therapy into comprehensive treatment plans.
The Foundations of Pelvic Floor Therapy for Common Conditions
Pelvic floor therapy is a non-invasive, evidence-based treatment that addresses a range of common conditions, including urinary incontinence and pelvic organ prolapse. For women searching for Pelvic Floor Therapy Fort Lauderdale, understanding how this specialized care works is the first step toward lasting relief. At Dr. Anghel OBGYN, we provide expert pelvic floor therapy in Fort Lauderdale to help women regain control and improve their quality of life.
Understanding the different types of urinary incontinence is essential to tailoring an effective treatment plan. According to the Office on Women's Health (U.S. Department of Health and Human Services), urinary incontinence is broadly categorized into three types: stress incontinence, urge incontinence, and mixed incontinence. Stress incontinence involves leakage during physical activity, while urge incontinence causes a sudden, intense need to urinate. Mixed incontinence combines symptoms of both. The following table summarizes the key characteristics, common triggers, and expected effectiveness of pelvic floor therapy for each type, helping patients understand their own symptoms and what to expect from treatment.
| Condition | Stress Incontinence | Urge Incontinence | Mixed Incontinence |
|---|---|---|---|
| Description | Leakage with physical activity | Sudden strong need to urinate | Combination of stress and urge |
| Common Triggers | Coughing, sneezing, exercise | Hearing running water, key in lock | Multiple triggers |
| Therapy Effectiveness | High with Kegels, biofeedback | Moderate with bladder training, therapy | Variable, often combination approach |
Research published by the National Center for Biotechnology Information confirms that pelvic floor muscle training (PFMT) yields significant improvement for stress and urge incontinence. For stress incontinence, Kegel exercises and biofeedback help strengthen the pelvic floor muscles, reducing leakage during coughing or exercise. Urge incontinence often responds to bladder training and behavioral strategies, helping to moderate sudden urges triggered by everyday sounds like running water. Mixed incontinence, which presents with both patterns, typically requires a customized, multimodal approach combining strengthening and bladder retraining. The APTA Pelvic Health Academy recommends consistent practice and gradual progression under a therapist's guidance to achieve the best outcomes.
Pelvic floor therapy is also highly effective for pelvic organ prolapse, providing support and symptom relief through targeted muscle strengthening and education on proper body mechanics.
Beyond incontinence and prolapse, pelvic floor therapy is a key component of pelvic pain management for many women.
Now that you understand the foundations, the next section explores how pelvic floor therapy is delivered in our Fort Lauderdale practice, where we provide the safest and most effective care to help every woman feel comfortable and confident at every stage of life.
Techniques and Expectations in Pelvic Floor Therapy
For women seeking relief from pelvic health concerns, Pelvic Floor Therapy in Fort Lauderdale offers a conservative, evidence-based treatment pathway that prioritizes patient comfort and functional recovery. This specialized form of physical therapy addresses the musculoskeletal structures that support the bladder, uterus, and bowel, helping patients regain control and confidence. Understanding what happens during a session demystifies the process and empowers women to take an active role in their healing journey.
What to Expect During Your First Pelvic Floor Therapy Appointment
We believe that expert and attentive care begins with a thorough understanding of your unique health history. Your initial evaluation typically lasts 60 to 90 minutes and starts with a detailed conversation about your symptoms, childbirth experiences, lifestyle habits, and specific goals. This dialogue allows the therapist to piece together the factors contributing to your condition, whether it's urinary incontinence, pelvic pressure, or postpartum healing. We then proceed to an external assessment, palpating the abdominal and pelvic girdle muscles to identify areas of tension, weakness, or asymmetry. If your evaluation suggests a need for additional specialized care, we offer comprehensive urogynecology services, including advanced diagnostics and surgical treatments, to ensure you receive the right level of support.
For many patients, an internal assessment provides the most precise information about pelvic floor muscle function. We explain the rationale for this step in detail and obtain your explicit consent before proceeding--you are always in control, and declining this portion will not compromise the quality of your care. The therapist uses a single, lubricated gloved finger to assess muscle tone, endurance, and coordination, and may provide gentle cuing so you can feel exactly which muscles to engage. The entire session is collaborative: together, we set functional goals that might include reducing leakage episodes, managing prolapse pressure, or returning safely to exercise. You are encouraged to ask questions at any point, and many patients share that they feel comfortable and confident knowing the therapist respects their boundaries.
According to guidelines from the American Physical Therapy Association (APTA) Pelvic Health, this thorough evaluation process ensures that each treatment plan is tailored to the individual, not the diagnosis. By the end of your first visit, you will have a clear understanding of the proposed therapy plan, the expected frequency of sessions, and the realistic timeline for improvement.
Manual Techniques, Biofeedback, and Electrical Stimulation
Once the assessment is complete, the therapist selects therapeutic modalities that match your specific needs, drawing on best practices outlined by professional organizations like APTA Pelvic Health. Manual techniques often form the foundation of care, particularly when muscles are hypertonic (too tight) or painful. The therapist applies gentle myofascial release to the abdominal wall, hips, and pelvic floor, working externally most often. Trigger point therapy targets specific knots within the pelvic muscles, while assisted stretching improves tissue mobility. These hands-on methods are non-invasive and focused on releasing tension so the muscles can contract and relax normally again.
For patients who struggle to identify or coordinate their pelvic floor contractions, biofeedback is an invaluable tool. Small, adhesive sensors are placed on the perineum or a slim vaginal sensor is inserted; these detect the electrical activity of your muscles and display the signal on a screen. Watching a graph rise and fall in real time as you contract and rest gives you visual confirmation that you are engaging the correct muscles--a powerful learning aid for those who have been performing Kegels incorrectly. Therapists may also introduce electrical stimulation, which delivers a low-current impulse via a specialized probe to help re-educate dormant or severely weak muscles. The sensation is mild and rhythmic, described by most patients as a gentle tingling that produces a visible muscle contraction.
These modalities are always adjusted to your tolerance, and you remain an active partner throughout. The American College of Obstetricians and Gynecologists (ACOG) notes that non-invasive strategies like biofeedback and stimulation are particularly effective when combined with behavioral modifications. At every stage of a woman's life--from the postpartum months through menopause--these tools can restore confidence and bladder control without the need for surgery.
Targeted Exercises for Stress Incontinence and Postpartum Recovery
Pelvic floor exercises are the cornerstone of treatment for urinary incontinence and postpartum rehabilitation. Clinical evidence from the National Center for Biotechnology Information (NCBI) demonstrates that a structured, progressive program can reduce leakage episodes by up to 75% in women with stress incontinence. The most well-known exercise is the Kegel, but proper technique is critical. We teach patients to "draw the pelvic floor up and in"--as if stopping the flow of urine and holding back gas simultaneously--without gripping the buttocks, thighs, or abdominal muscles. Quick flick contractions build fast-twitch fibers that clamp the urethra during a cough or sneeze, while endurance holds (10-second squeezes) develop the slow-twitch fibers needed for sustained support throughout the day.
Postpartum recovery demands an integrated approach that goes beyond Kegels alone. The transversus abdominis--the deepest layer of abdominal muscle--works in synergy with the pelvic floor to stabilize the core. We teach a gentle drawing-in maneuver combined with diaphragmatic breathing: on the inhale, the belly and pelvic floor soften; on the exhale, the navel draws toward the spine and the pelvic floor gently lifts. Patients progress through positions only when they can maintain this coordination: starting lying down, advancing to sitting on a stability ball, and finally integrating the contraction into standing activities like lifting a child.
Consistency is more important than intensity. We recommend short, frequent practice sessions rather than long, exhausting workouts. By incorporating these exercises into daily routines--such as performing holds while feeding the baby or quick flicks at red lights--patients build lasting habits. Many women report significant benefit, with improvements in both symptom severity and overall quality of life, as long as they continue practicing under periodic therapist guidance.
Comparison of treatment pathways helps patients understand where physical therapy fits within the spectrum of care for pelvic support disorders. The following table summarizes the key differences between non-surgical pelvic floor therapy and surgical approaches for managing pelvic organ prolapse, drawing on recommendations from APTA, NCBI, and ACOG.
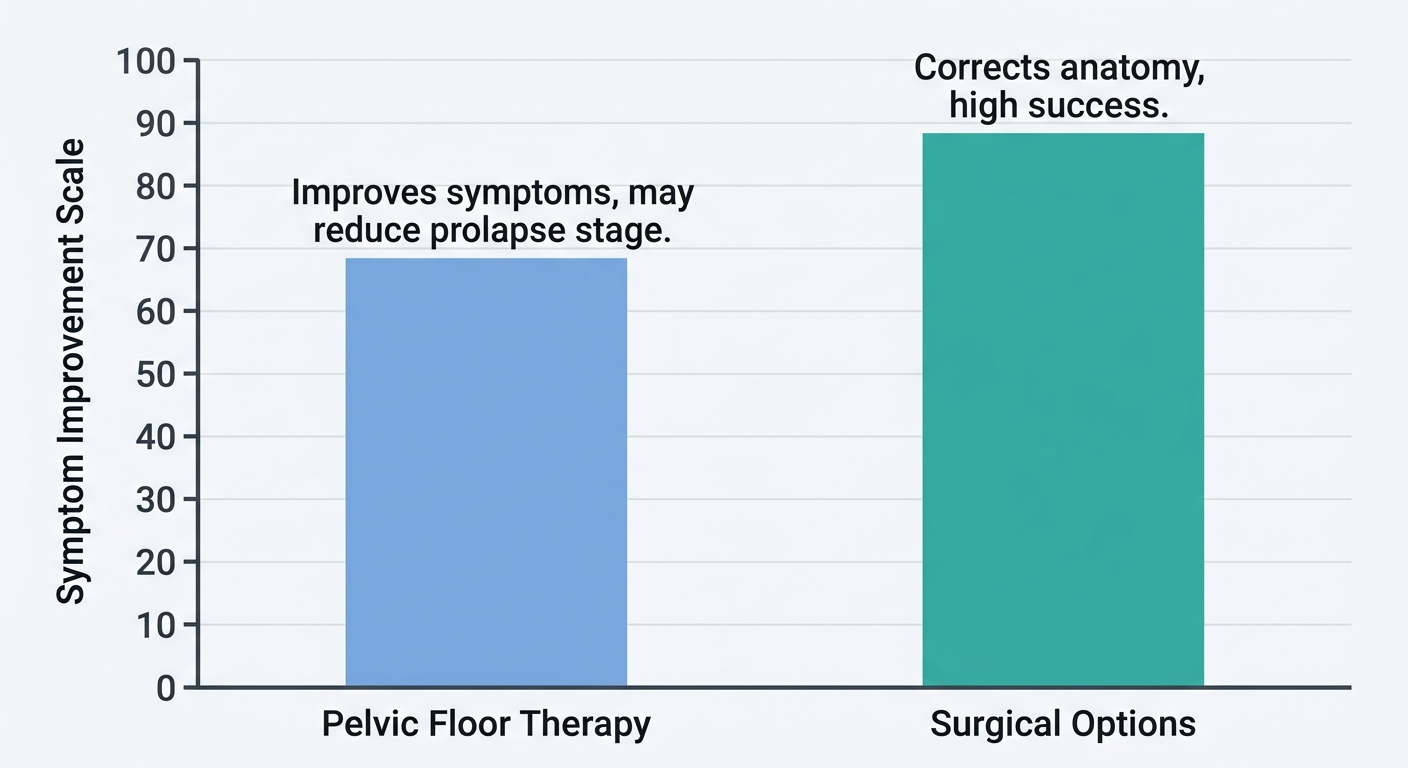
Effectiveness comparison: pelvic floor therapy vs. surgical options
Reviewing the data, it becomes evident that pelvic floor therapy serves as an excellent first-line option for women with mild-to-moderate prolapse who wish to avoid intervention. Surgical repair, including robotic procedures and pessary fitting, is appropriately reserved for advanced stages or when symptoms severely impact daily living--scenarios where anatomical correction offers the most durable resolution. With these techniques in mind, let's explore how therapy fits into a comprehensive care plan.
Steps to Begin Your Pelvic Floor Therapy Journey in Fort Lauderdale
Once you recognize the signs of pelvic floor dysfunction, the next step is understanding how to begin your therapy journey. If you're seeking effective Pelvic Floor Therapy in Fort Lauderdale, our practice at First Class OBGYN provides expert and attentive care tailored to your unique needs. Whether your symptoms point toward conservative pelvic muscle therapy or require a combined urogynecologic approach, we guide you from initial evaluation through every milestone.
When to Seek a Urogynecologist for Pelvic Floor Issues
Many women find that mild urinary incontinence or early-stage pelvic organ prolapse responds well to pelvic floor rehabilitation alone. However, clinical practice guidelines from the American College of Obstetricians and Gynecologists (ACOG) indicate that certain situations call for a urogynecologist's involvement--such as advanced prolapse, mixed conditions that don't improve with therapy alone, or failure to achieve meaningful symptom relief after a dedicated course of conservative care. At our Fort Lauderdale practice, we help you decide at the outset which path offers the safest and most effective care for your circumstances.
The following table summarizes the key differences between pursuing pelvic floor therapy alone and adding urogynecologic interventions.
| Aspect | Non-Surgical (Pelvic Floor Therapy) | Surgical Options (Pessary, Surgery) |
|---|---|---|
| Effectiveness for Prolapse | Improves symptoms, may reduce prolapse stage in mild cases | Corrects anatomy, high success for advanced prolapse |
| Invasiveness | Non-invasive | Minimally invasive to open surgery |
| Recovery Time | No downtime | Days to weeks |
| Cost Consideration | Lower upfront cost | Higher upfront cost |
As the table illustrates, patients with mild-to-moderate urinary incontinence or uncomplicated prolapse often achieve substantial improvement through consistent pelvic floor rehabilitation alone. When symptoms are more complex, however, combining therapy with advanced urogynecologic procedures can deliver more comprehensive results. Our team, led by a board-certified urogynecologist with expertise in da Vinci robotic-assisted surgery, ensures that you receive world-class urogynecological care--whether you need conservative treatment or the least invasive gynecologic surgery available.
With a clear picture of when urogynecologic expertise is needed, the next focus is developing your personalized treatment roadmap.
Pelvic floor therapy patient journey visualization
Creating a Customized Treatment Plan: Sessions and Milestones
At First Class OBGYN, we design every treatment plan to help you feel comfortable and confident from your very first visit. According to professional practice standards from the American Physical Therapy Association (APTA), pelvic floor therapy sessions are typically scheduled one to two times per week, with initial functional improvements often measurable within 8 to 12 weeks. Research published by the National Center for Biotechnology Information (NCBI) supports this timeline, showing that consistent, guided rehabilitation leads to meaningful gains in muscle strength and symptom control.
Your plan is built around clear, measurable milestones that we track together:
- Improved pelvic floor muscle strength and endurance during internal assessments.
- Reduction in the number of urinary leakage episodes per day.
- Decreased pelvic pressure or discomfort when standing or lifting.
- Restored ability to participate in exercise, work, and daily activities without fear of incontinence.
- Enhanced pelvic organ support, reducing the sensation of prolapse.
Consistency is the foundation of success, and our highly skilled and warm team works with you to schedule sessions that fit your life. We also handle insurance verification, confirming that a physician referral is in place so your therapy is covered under your plan--without adding financial stress. For patients who need combined care, we coordinate seamlessly between your physical therapist and our urogynecology team to deliver cohesive treatment.
After establishing your plan, we remain by your side through every session, tracking your progress and adjusting your approach so you can move forward with renewed confidence.
Advanced Interventional Options for Pelvic Floor Disorders
When pelvic floor therapy alone does not provide sufficient relief, we offer advanced interventional options tailored to each patient's needs. For women who have completed pelvic floor therapy in Fort Lauderdale and still experience symptoms, our practice provides a spectrum of minimally invasive procedures.
These procedures are recommended only after conservative therapy has not yielded adequate results, as outlined by the American Physical Therapy Association - Pelvic Health Section. Recovery timelines, supported by evidence from the National Center for Biotechnology Information, vary from immediate return to normal activities with MonaLisa Touch to a few weeks for robotic surgery.
We offer robotic sacrocolpopexy, a minimally invasive surgical option for women with advanced pelvic organ prolapse. The procedure leverages the benefits of robotic surgery, including tiny incisions, minimal scarring, reduced post-operative discomfort, faster return to daily life, and a 2- to 4-week recovery. We typically recommend this when conservative measures such as pelvic floor therapy in Fort Lauderdale have not fully resolved the condition.
For vaginal atrophy and dryness, we offer the MonaLisa Touch laser system, a minimally invasive in-office treatment that stimulates collagen production and restores vaginal tissue without hormones. There is no required downtime, so patients can immediately return to their daily routines. Many women find that pairing this treatment with pelvic floor therapy enhances results by addressing both muscular weakness and tissue health.
For overactive bladder and urinary incontinence that persists after conservative treatment, we provide InterStim neuro-modulation therapy. This Medtronic device is implanted in a short procedure with 1-2 days of recovery. It works by sending mild electrical pulses to the sacral nerves, helping to regulate bladder function and significantly reduce symptoms. Research supports its effectiveness for refractory cases, and our patients experience improved control and quality of life.
Our vaginal rejuvenation procedures, including labiaplasty and vaginoplasty, are tailored to address both cosmetic and functional concerns like laxity, discomfort, or reduced sensation. Using advanced, least invasive techniques, patients can expect a 1- to 2-week recovery. This elective option can improve self-esteem and sexual function, and may be integrated into a comprehensive treatment plan alongside pelvic floor therapy. We ensure every patient feels comfortable and confident in her choice with personalized consultations.
At First Class OBGYN, we combine pelvic floor therapy with advanced, least invasive surgical options to deliver the safest and most effective care. Our expert and attentive care ensures every patient feels comfortable and confident knowing we tailor treatments to her unique needs.
Frequently Asked Questions About Pelvic Floor Therapy
We've covered the key aspects of pelvic floor therapy; now, here are answers to common questions.
What is pelvic floor therapy and what conditions does it treat? Pelvic floor therapy strengthens the pelvic muscles and effectively treats urinary incontinence, pelvic organ prolapse, and other disorders. According to the Office on Women's Health, U.S. Department of Health and Human Services, these conditions affect millions of women and respond well to rehabilitation. Our pelvic floor therapy in Fort Lauderdale includes biofeedback and personalized exercises.
Can pelvic floor therapy help with endometriosis? Yes, it can reduce pelvic muscle tension and pain associated with endometriosis. For comprehensive management, explore our dedicated information on Endometriosis Fort Lauderdale.
How do I get started with pelvic floor therapy? Contact our Miramar office to schedule a consultation. We provide the safest and most effective care, so you can feel comfortable and confident starting your journey. If you're ready to begin pelvic floor therapy in Fort Lauderdale, our team is here to help.
Take Charge of Your Pelvic Health with Expert Care
Take charge of your pelvic health with Pelvic Floor Therapy Fort Lauderdale patients trust at First Class OBGYN, where we combine advanced expertise with compassionate care in Fort Lauderdale. Whether you are managing pelvic organ prolapse or urinary incontinence, our board-certified team offers expert and attentive care, utilizing advanced, least invasive gynecologic surgery including da Vinci robotic techniques. We ensure you feel comfortable and confident, drawing on high-risk pregnancy expertise and multilingual support. Take the next step toward lasting relief -- schedule your consultation with us today.
This article was researched and written with the assistance of AI tools.














