Table of Contents
Hormone Replacement Therapy in Pembroke Pines, Florida: A Complete Guide
For women in Pembroke Pines considering hormone replacement, hormone replacement therapy (HRT) offers a proven path to manage disruptive menopause symptoms. HRT supplements the body with estrogen and progesterone, effectively relieving hot flashes, night sweats, vaginal dryness, and mood swings. When customized by a knowledgeable physician, this therapy can deliver significant menopause symptom relief and help protect against long-term bone loss. HRT can also improve sleep quality and overall well-being, making daily life more comfortable.
Two primary types of hormones are used in treatment: synthetic hormones and bioidentical hormones. Synthetic hormones are FDA-approved and have been extensively tested for safety and efficacy. Bioidentical hormones, which are chemically identical to the body's own hormones, are available in FDA-approved forms, but compounded bioidentical hormone therapy products are not FDA-reviewed. As the U.S. Food and Drug Administration (FDA) cautions, these unregulated compounds may pose unknown risks. Government health authorities, including the Office on Women's Health, recommend using the lowest effective dose for the shortest time necessary and regular follow-up.
Dr. Anghel OBGYN in Pembroke Pines provides expert Hormone Therapy Pembroke Pines as part of our comprehensive menopause care. We craft personalized treatment plans that follow the latest clinical guidelines, prioritizing safety and regular monitoring. In the following sections, we will explore the different types of HRT available and their specific benefits. Contact our office in Pembroke Pines to learn more about hormone replacement therapy and find relief from menopause symptoms.
Understanding Hormone Replacement Therapy: Types and Mechanisms
Hormone replacement therapy (HRT) provides much-needed relief from menopause symptoms such as hot flashes, night sweats, and mood swings. For women in the Pembroke Pines area, learning about the two primary categories--traditional synthetic HRT and bioidentical hormone therapy--can help guide personalized treatment decisions. The table below highlights the key differences, illustrating how they vary in source, structure, regulation, and typical use.
| Aspect | Traditional HRT | Bioidentical Hormone Therapy |
|---|---|---|
| Source | Synthetic hormones (e.g., Premarin from pregnant mares' urine) | Plant-derived hormones chemically identical to human hormones |
| Molecular Structure | May differ from human hormones structurally | Exact replicas of human estradiol, progesterone, and testosterone |
| Customization | Fixed-dose preparations (standardized) | Compounded individually based on blood/saliva levels |
| FDA Regulation | FDA-approved and monitored | Mostly FDA-approved (e.g., patches, gels); compounded forms regulated at state level |
| Typical Use | Short-term menopause symptom relief | Often used for long-term, individualized balance |
According to the Cleveland Clinic, bioidentical hormone therapy uses hormones derived from plant sources that are chemically identical to those produced by the human body, including estradiol, progesterone, and testosterone. In contrast, traditional HRT often relies on synthetic hormones like conjugated equine estrogens (e.g., Premarin, derived from pregnant mares' urine), which may differ structurally from endogenous hormones. Because bioidentical hormones share the exact molecular structure of endogenous hormones, they bind to the same cellular receptors in the same way, mimicking natural physiological activity. Synthetic hormones can still exert hormonal effects but may interact with receptors with slightly different affinities, potentially leading to distinct side-effect profiles. Hormone level testing--through blood or saliva--is typically performed before customizing a bioidentical regimen, ensuring that the therapy matches the woman's specific deficiencies.
As the table makes clear, the two approaches diverge sharply in customizability and oversight. Traditional HRT provides standardized, FDA-approved preparations that are effective for short-term menopause symptom relief. Bioidentical therapy introduces personalized dosing based on an individual's hormone profile, often attracting women who are interested in longer-term, balanced care. WebMD notes that this personalization, grounded in laboratory assessments, is a defining advantage of compounded bioidentical hormones.
Customization is a key differentiator: bioidentical hormones are frequently compounded after testing blood or saliva levels, whereas traditional HRT comes in fixed doses. In terms of regulation, all traditional HRT medications are FDA-approved and monitored, while bioidentical therapy includes both FDA-approved forms--such as transdermal patches and gels--and compounded preparations that fall under state pharmacy oversight, as highlighted by the Cleveland Clinic. This regulatory distinction can influence the perception of safety. Typically, traditional HRT is prescribed for short-term menopause symptom relief to limit potential risks, while bioidentical therapy is often chosen by women pursuing long-term, individualized hormone balance.
At First Class OBGYN, we provide expert and attentive care for every stage of a woman's life, including menopause management. Understanding the differences between traditional and bioidentical HRT is crucial when evaluating potential benefits and risks. For women in Pembroke Pines seeking personalized treatment, Hormone Replacement Therapy Pembroke Pines offers both options tailored to individual needs.
Bioidentical Hormone Therapy: How It Works and What to Expect
For women in Pembroke Pines exploring Hormone Replacement Pembroke Pines, bioidentical hormone therapy provides a personalized path to menopause symptom relief. At First Class OBGYN, we believe that every woman deserves a treatment plan tailored to her unique hormonal balance. This section explains how bioidentical hormones work, the various delivery methods available, and what you can expect throughout your therapy.
The Science Behind Bioidentical Hormones
According to the Cleveland Clinic, bioidentical hormones are man-made compounds with a molecular structure identical to the hormones your body produces naturally--such as 17β-estradiol, progesterone, and testosterone. Because these compounds replicate your endogenous hormones exactly, they bind to hormone receptors in the same way, potentially providing effective relief for perimenopausal and menopausal symptoms. Unlike conventional synthetic HRT, which uses hormones that are not chemically identical to human hormones, bioidentical hormone therapy often relies on compounding pharmacies to create customized doses based on your individual lab results. This individualized approach allows us to address your specific hormonal deficiencies rather than applying a one-size-fits-all solution. Many women prefer this personalized HRT because it aims to restore balance with substances their bodies already recognize. This personalized, natural-identical hormone therapy has gained popularity among women seeking menopause relief without synthetic substitutes. The goal is to achieve symptom relief while using the lowest effective dose, and because the hormones are bioidentical, they are metabolized by the body just like natural hormones.
Delivery Methods and Treatment Plans
Bioidentical hormones are available in several formulations, each designed to meet different needs. Subdermal pellets are placed under the skin in a quick in-office procedure and release hormones steadily for three to six months, requiring minimal effort. Transdermal creams are applied daily, offering at-home control and the ability to fine-tune dosing. Patches, changed twice weekly or weekly, deliver a consistent hormone release through the skin, while injections (administered weekly to monthly) can provide stronger, targeted therapy. The table below compares these options in detail:
| Method | Frequency | Pros | Cons | Ideal For |
|---|---|---|---|---|
| Subdermal Pellets | Every 3-6 months | Consistent hormone levels, minimal user effort | Requires minor in-office insertion procedure | Patients who prefer long-term, low-maintenance therapy |
| Transdermal Creams | Daily application | Easy to adjust dose, avoids first-pass liver metabolism | Possible skin irritation, variability in absorption | Patients who want flexibility and at-home control |
| Patches | Twice weekly or weekly | Steady hormone release, FDA-approved options | May cause skin reactions, less dose customization | Patients seeking convenience and stable levels |
| Injections | Weekly to monthly | Rapid absorption, effective for specific hormones | Peaks and troughs, requires office or self-injection | Patients who need targeted or higher-dose therapy |
Selecting the ideal delivery method is a personal decision. Some women prefer the convenience of long-acting pellets, while others value the flexibility of daily creams. We take the time to discuss the pros and cons of each, helping you find the approach that fits your routine. We consider your hormone levels, medical history, and lifestyle preferences when recommending a method. Our goal is to make you feel comfortable and confident with your treatment plan. FDA-approved patches are another reliable choice for those who want steady release without daily applications. Once treatment begins, we'll monitor your response and adjust as needed--a topic covered in the next section.
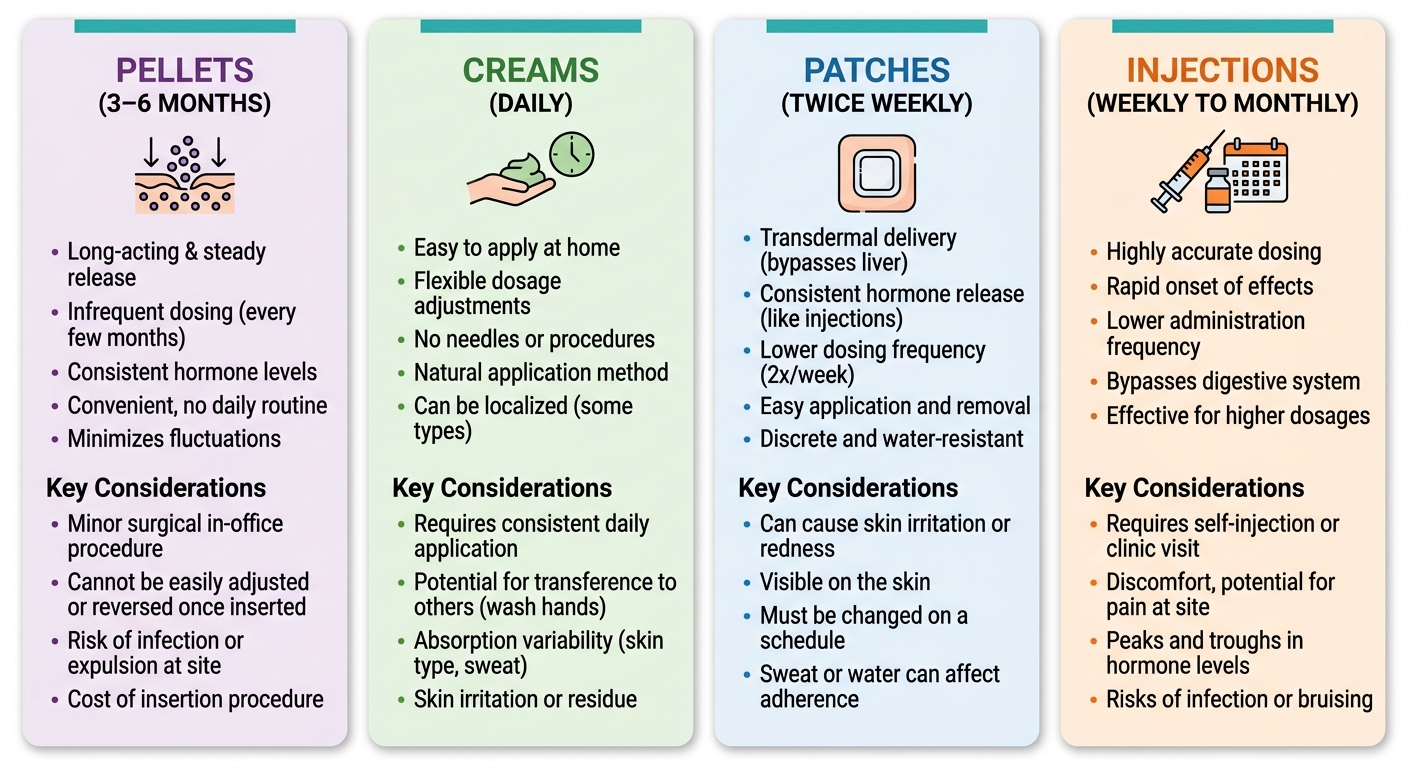
Comparison chart of four bioidentical hormone therapy delivery methods.
When you're ready to explore hormone replacement therapy Florida, our team is here to provide care that adapts as your needs change.
Monitoring and Adjusting Your Therapy
Ongoing monitoring is a cornerstone of safe and effective bioidentical hormone therapy. After starting treatment, we schedule follow-up visits--typically every three to six months--to assess your symptom relief and overall well-being. During these visits, we may use blood or saliva testing to evaluate your hormone levels and ensure they are within the optimal therapeutic range. Based on your results and any lingering symptoms, we may adjust your dosage or delivery method. This personalized, iterative approach allows us to fine-tune your therapy to achieve maximum benefit with the lowest possible dose. Our team at First Class OBGYN is committed to supporting you throughout every stage of your journey, making adjustments as your body changes. We also recommend periodic bone density screenings and cardiovascular assessments as part of your comprehensive menopause care, because hormone changes can affect more than just mood and hot flashes. This holistic monitoring ensures we address your overall health while optimizing your hormone therapy. Regular communication helps us catch any imbalances early and maintain your quality of life. We encourage you to share any new symptoms or concerns promptly, so we can modify your plan in real time. With consistent follow-up, we help you navigate this phase of life with confidence.
Finding Menopause Symptom Relief with Personalized Care in Pembroke Pines
Women exploring hormone replacement in Pembroke Pines deserve a personalized, evidence-based approach that addresses both the symptoms and root causes of menopause. At First Class OBGYN, we combine advanced medical therapies with holistic lifestyle strategies to deliver comprehensive care for every woman.
At First Class OBGYN, we offer comprehensive menopause treatment Florida, tailored to your needs in Pembroke Pines. The journey to effective menopause symptom relief follows three key steps, as shown in the process below.
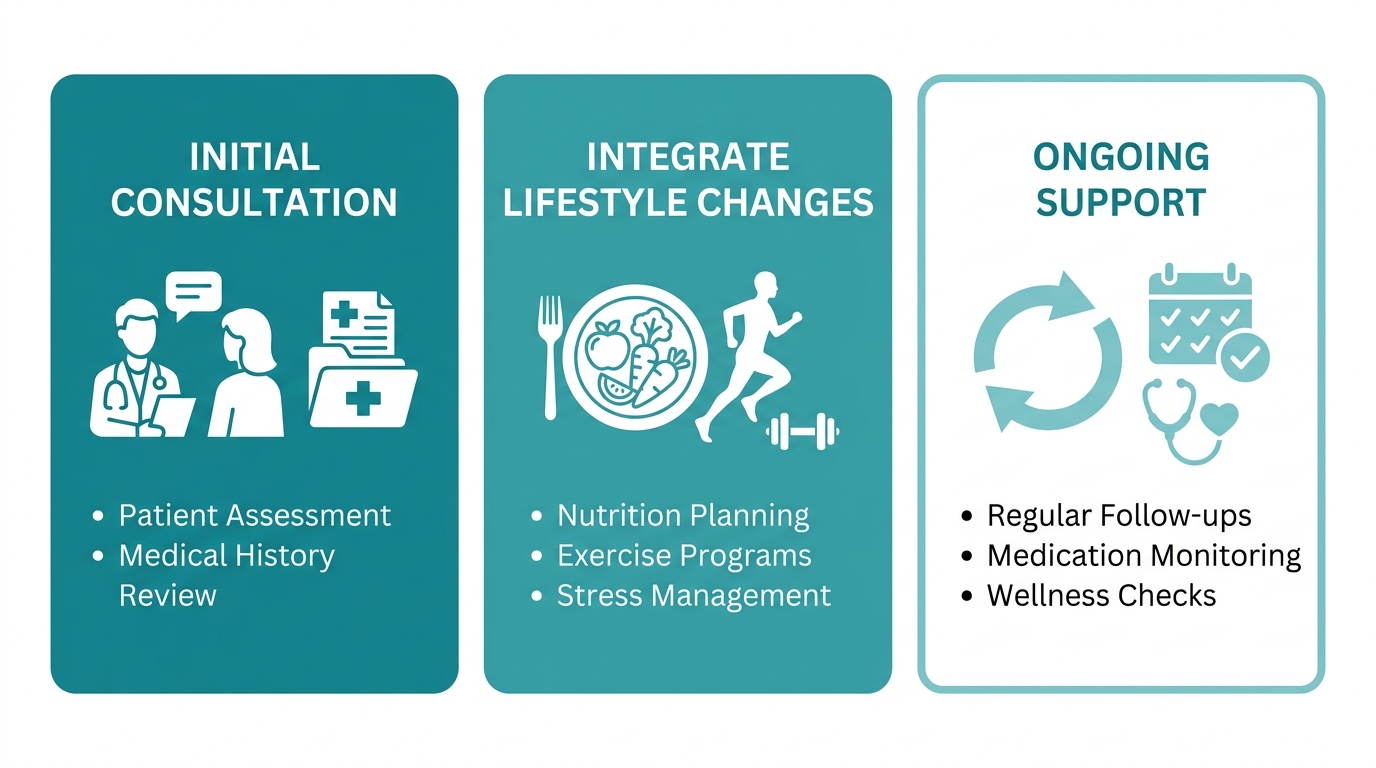
Personalized menopause symptom relief journey in three clear steps
Our team, led by board-certified OB-GYN Dr. Laviniu Anghel, guides you through each phase with expert and attentive care, ensuring you feel comfortable and confident at every stage of a woman's life.
Initial Consultation and Candidacy Evaluation
Your first visit establishes the foundation for safe, individualized treatment. We ask you to bring your insurance card, a complete list of medications, and, if possible, a symptom diary tracking hot flashes, sleep quality, and mood changes over two weeks. A thorough health history review includes family history of breast cancer and heart disease, as these can influence therapy choices.
Symptom severity is assessed using validated tools like the Menopause Rating Scale, giving us an objective baseline. We then order targeted lab tests -- FSH, estradiol, TSH, a lipid panel, and hemoglobin A1c -- to uncover any metabolic or thyroid contributors to your symptoms. Dr. Anghel evaluates your cardiovascular risk, breast cancer risk, and personal preferences to determine whether hormone therapy is appropriate. For many women, bioidentical hormone therapy is tailored to match each individual's hormonal profile, offering a precise path to relief.
Integrating Lifestyle Changes for Optimal Results
Medication is only part of the equation. We prescribe lifestyle modifications that work synergistically with HRT to enhance benefits and reduce risks. A diet rich in phytoestrogens -- found in soy, flaxseed, and legumes -- can help modulate hormone activity. We recommend daily calcium intake of 1,200 mg and vitamin D of 600-800 IU to protect bone density. Regular physical activity, at least 150 minutes per week combining aerobic and weight-bearing exercises, supports cardiovascular and metabolic health.
Stress management techniques such as mindfulness, yoga, or simple breathing exercises lower cortisol levels, which can worsen hot flashes. Limiting alcohol and caffeine also helps stabilize temperature regulation. For optimal menopause symptom relief, we emphasize that combining HRT with these lifestyle habits yields the most consistent and lasting improvements.
The table below compares the three main approaches to managing menopause symptoms:
| Approach | Symptom Relief | Safety Profile | Long-Term Benefits | Patient Effort |
|---|---|---|---|---|
| HRT Alone (Traditional or Bioidentical) | Highly effective for hot flashes, night sweats, vaginal dryness | Requires individualized dosing; risk of blood clots, breast tenderness | Can preserve bone density, improve mood and sleep | Moderate: adherence to dosing schedule and monitoring |
| Lifestyle Modifications Only | Mild to moderate; may take weeks to notice improvement | Very safe; minimal side effects | Improves overall health, weight management, cardiovascular fitness | High: requires consistent dietary changes, exercise, stress management |
| Combined HRT + Lifestyle | Optimal; addresses both hormone deficiency and overall well-being | Careful monitoring balances effectiveness and risk | Synergistic effects on bone, heart, and mental health | Moderate to high: requires commitment to both treatment and habits |
According to the Office on Women's Health, combination HRT may be prescribed when both estrogen and progesterone are needed, and careful monitoring can balance benefits with potential risks. We also advise targeted supplements like magnesium for sleep or vitamin E for hot flashes, always under our guidance. By pairing expert medical oversight with everyday habits, patients experience a greater sense of control and vitality.
Ongoing Support and Follow-Up Visits
After starting therapy, we schedule follow-up visits at 3 months, 6 months, and then annually. At each appointment, you will review a symptom diary and repeat key labs -- serum estradiol, SHBG, and others -- to gauge your response. Based on this data, Dr. Anghel may adjust your HRT, for instance shifting from oral estradiol to a transdermal patch or modifying the progesterone dose to minimize side effects.
Our multidisciplinary team -- including nurses and a nutritionist -- works together to provide seamless support. Dr. Anghel's Fellowship from the American College of Obstetricians and Gynecologists and her ability to communicate fluently in English, Spanish, and Romanian ensure personalized, culturally sensitive care. With a solid care plan in place, our patients often find that their symptoms improve significantly, allowing them to focus on overall wellness.
Long-Term Health Considerations and Future Directions in Hormone Therapy
For women exploring hormone replacement in Pembroke Pines, the duration of therapy is a critical factor in balancing benefits and potential risks. While short-term use (1-5 years) is well-documented for providing rapid menopause symptom relief, the decision to extend treatment beyond five years demands careful, individualized evaluation.
| Duration | Primary Benefits | Common Concerns | Monitoring Needs |
|---|---|---|---|
| Short-term (1-5 years) | Rapid relief of vasomotor symptoms, improved sleep and quality of life | Risk of blood clots, breast tenderness, possible weight gain | Annual check-ups, symptom tracking, periodic lab work |
| Long-term (5+ years) | Sustained symptom management, bone density preservation, potential cardiovascular protection | Increased breast cancer risk (with combined therapy), need for dose adjustment | More frequent visits, advanced biomarker testing, individualized protocol adjustments |
The table above highlights key distinctions. Short-term therapy focuses on quickly easing hot flashes and night sweats, enabling many women to feel like themselves again with minimal monitoring. In contrast, long-term hormone replacement often preserves bone density and may offer heart health advantages when started near menopause, yet it also introduces concerns such as a documented rise in breast cancer risk with combined estrogen-progestin regimens. Estrogen-only treatment, however, appears to carry a lower risk profile. This is why we transition long-term patients to more frequent evaluations and advanced biomarker testing to ensure the safest and most effective care possible.
Looking ahead, the future of hormone therapy lies in precision medicine and novel delivery methods. The U.S. Food and Drug Administration (FDA) underscores that compounded bioidentical hormone therapy products are not subject to the same rigorous testing as approved medications, reinforcing our practice's commitment to evidence-based protocols. As personalized care becomes the gold standard, we encourage patients to explore our full range of obgyn services south florida for integrated women's health. For those seeking extended menopausal treatment in Pembroke Pines, our team tailors every plan to evolving needs, adjusting doses and formulations to optimize safety and long-term well-being.
By combining thorough monitoring with compassionate guidance, we remain dedicated to delivering expert and attentive care at every stage of a woman's life.
Common Questions About Hormone Replacement Therapy in Pembroke Pines
Hormone replacement therapy in Pembroke Pines raises several common questions, and our team is here to help. HRT replaces hormones that decline during menopause, using either systemic estrogen or low-dose vaginal therapies for local symptoms, as described by the Office on Women's Health. Bioidentical hormones, which the Cleveland Clinic defines as structurally identical to the body's own hormones, are one type of HRT. This bioidentical hormone therapy can provide effective menopause symptom relief--reducing hot flashes, night sweats, and vaginal dryness--while also helping to preserve bone density. However, the same government source highlights risks including blood clots, breast cancer, and heart disease; these risks are lowest when therapy is started within 10 years of menopause. For women in Pembroke Pines, we offer personalized hormone evaluations and compassionate guidance through every stage of a woman's life. For expert and attentive care, turn to First Class OBGYN Women's Health, your partner in hormone therapy management.
Your Journey to Hormonal Balance and Better Well-Being
Achieving hormone replacement in Pembroke Pines is a vital step toward restoring hormonal balance and improving overall well-being. Our practice provides bioidentical hormone therapy, offering menopause symptom relief from hot flashes, night sweats, and mood swings. As advised by Cleveland Clinic, we prioritize safety and personalized care, creating customized plans for each woman. With expert and attentive care through every stage of a woman's life, we guide you toward renewed vitality. Schedule your consultation with Dr. Anghel today to start your journey.
This article was researched and written with the assistance of AI tools.














